The bereavement services team at Heartlands Hospital has won the prestigious ‘Best Hospital Care’ award at the 2013 Butterfly Awards, having cared for more than 1,600 families in Birmingham which have experienced the loss of a baby.
The bereavement services team at Heartlands Hospital has won the prestigious ‘Best Hospital Care’ award at the 2013 Butterfly Awards, having cared for more than 1,600 families in Birmingham which have experienced the loss of a baby.
The Butterfly Awards celebrate the achievements of the healthcare professionals that support families during this difficult time.
Established in 2004, the bereavement services team provides a holistic service, from the time a family is bereaved, to the birth, funeral, follow-up appointments, ongoing support and help when planning future pregnancies. The Heart of England NHS Foundation Trust has two dedicated bereavement suites at Heartlands – Eden and Snowdrop – to create a home-from-home environment, enabling families to have the time and space they need with their babies.
Clare Beesley, bereavement support midwife, said: “We are absolutely delighted to win ‘Best Hospital Care’ at the 2013 Butterfly Awards, and would like to thanks all those who voted for us. Receiving this kind of recognition is truly heart-warming. We work hard to provide a service of the highest standard to parents and families going through the loss of a baby, and to be recognised for delivering the best hospital care for bereaved parents in the country is wonderful.
“We take pride in the fact that our team is trained to offer compassionate care and support, in a ‘home-from-home’ environment where families can spend time with their babies and create memories that will last a lifetime. By working closely with user groups and the local community, we will continue to develop our service to meet the individual needs of each family, every time. At the heart of our care is the six C’s as highlighted by the chief nursing officer for England: care, compassion, courage, competence, communication and commitment.
“Experiencing the loss of a child is one of the most difficult situations anyone can go through. The care and support we can offer to help carry families through these hard times makes a world of difference, and it means so much to win this award in recognition of all our hard work.”
Many people from across Birmingham vouched for the exceptional care received from the bereavement services team. Katie Pickett from Solihull received care and support following the loss of her son. She commented: “They helped us get through such a difficult time and made it as nice as it could be. All of the staff were so kind and caring, and made us feel at home. Without their kind nature, we wouldn’t have been able to spend quality time with our son or have the special memories that we have. They took copies of his footprints and locks of his hair – it was just so special to us. I think this enabled us to cope with the loss of our baby, and the team should be really proud of themselves.”
The daughter of Paul Warwick, from Yardley, also received help from the bereavement services team at Heartlands Hospital following the loss of her baby girl. He said: “The loss was absolutely devastating. All the nurses were outstanding, I couldn’t fault them. Time was never an issue to them – they would go home and come back in their own time, just to make sure we were OK. The service was just phenomenal.”
Around 2.9 million people living in the UK have diabetes, with an additional 850,000 people estimated to be living undiagnosed with the condition.
Birmingham has the highest rate of diabetes in the country, with nearly one in 10 people in some parts of the city living with the condition. Nearly 9.3 percent of the residents living in areas such as in Balsall Heath and Bordesley Green have diabetes according to the August 2013 statistics from the Health and Social Care Information Centre.
There are two main types – Type 1 diabetes and Type 2 diabetes. In both cases the symptoms are similar and will include an increased desire to drink as a result of being frequently thirsty, feeling very tired, losing weight and muscle bulk, and needing to urinate a lot, especially at night.
Type 1 diabetes can develop very quickly, in a matter of days or weeks. Around 10 percent of those diagnosed with diabetes will have Type 1 and it often shows itself when people are in their teens or before the age of 40.
Where Type 1 diabetes is present, the body is attacking and destroying insulin supplies, which results in there being no insulin produced. As a result, glucose remains in the blood and this can seriously harm internal organs.
If you are diagnosed with Type 1 diabetes, how can you manage the condition? Health and diet are vital and regularly monitoring your glucose levels will also help.
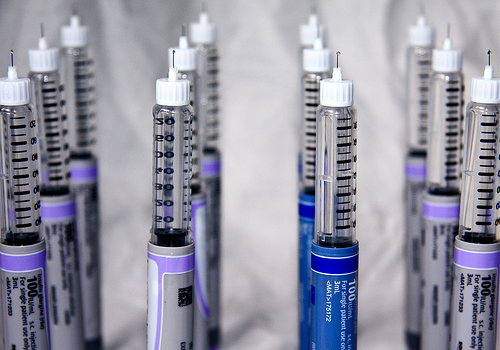
To keep your glucose levels normal, you may need regular insulin treatment. This mainly comes in the form of insulin injections. Injections can either be given with a syringe or an injection pen.
Type 2 diabetes is much more common than Type 1 diabetes. Type 2 is also known as ‘maturity onset’ diabetes and usually develops later in life.
Where Type 2 diabetes is present, the body either does not produce the required amount of insulin, or the body’s cells simply don’t respond to the insulin, resulting in insulin resistance.
Treating Type 2 diabetes is usually achieved through lifestyle choices, such as regular monitoring of blood glucose, as well as having a healthy and balanced diet. However this is a progressive form of the disease and may eventually result in the need for medication – usually in tablet form. Some people with Type 2 diabetes will also need insulin injections.
Dr. Jayadave Shakher, consultant diabetologist at Heartlands Hospital, believes there are two ways in which both types of diabetes can be prevented: “Eat healthily and avoid eating junk food as well as high sugar foods. Eating high sugar foods can lead to obesity and diabetes. Having fresh fruit and vegetables will make a difference.
“The second way you can prevent diabetes is by exercising regularly. Studies have shown the more outdoor activities you do; the more likely it is that the disease will decrease.”
There is also one additional form of diabetes that is specific to pregnant women – gestational diabetes. This affects around 5 percent of pregnant women and occurs where there are such high levels of glucose in the body during the pregnancy, that there simply isn’t enough insulin to deal with it.
Gestational diabetes will usually develop in the second trimester of pregnancy (weeks 14-26). There is a risk to the health of the unborn baby, as well as an increased chance of the mother developing Type 2 diabetes later in life. It is important to keep blood sugar levels under control where gestational diabetes develops.
If you have a family history of diabetes, make sure you see your GP. For more advice and information on diabetes, visit www.nhs.uk.

Karen McMullen (left), immunisation nurse, and Sarah Gill, immunisation team leader, at Solihull Community Services.
Significantly more girls aged between 12 and 13-years-old in Solihull are receiving the human papillomavirus (HPV) vaccine than the national average, offering vital protection against cervical cancer.
Between September 2011 and August 2012, 91.1 per cent of 12 to 13-year-olds received the vaccination in Solihull, compared to 86.8 per cent in England and 87.8 per cent in the West Midlands.
Uptake for the vaccination is greater in Solihull than a number of other nearby areas, including Walsall (86.8), Wolverhampton (84.1), Dudley (90.7) and Sandwell (88.4). The results are based on girls that have received all three doses of the HPV vaccine, which is injected over a 12-month period.
HPV is a common infection and is easily spread by sexual activity. As much as half of the population will be infected at some point in their life, but most cases can be controlled by a person’s immune system. However, in some cases the infection will persist and lead to a range of health problems, including cervical cancer.
According to Cancer Research UK, cervical cancer is the second most common cancer in women under the age of 35. Approximately 2,900 women are diagnosed with cervical cancer every year, and it has been estimated that 400 lives could be saved every year in the UK as a result of the vaccination programme.
Sarah Gill, HPV immunisation team leader at Solihull Community Services, said: “It is extremely encouraging to see that more than nine out of every ten girls aged between 12 and 13-years-old in Solihull are receiving the HPV vaccine, an essential vaccination that protects against cervical cancer. We endeavour to continue delivering this important vaccination programme to girls in Solihull.”
For more information on the HPV vaccine, please call 0121 744 0724.
The CQC is the independent regulator of all health and social care in England. We have been given powers by the government to register, monitor and inspect all health and care services.
The Care Quality Commission (CQC) will soon carry out an inspection at Heart of England NHS Foundation Trust, which covers Birmingham Heartlands Hospital, Solihull Hospital and Community Services , Good Hope Hospital and Birmingham Chest Clinic.
Tell us what you think about these hospitals by attending one of our listening events:
- Tuesday 12 November – Fellowship Community Hall, Sutton Coldfield, B72 1QU. 6.30pm start.
- Wednesday 13 November – Khidmat Centre, 2A Heather Road, Small Heath, B10 9TA. 7.00pm start.
- Thursday 14 November – National Motorcycle Museum, B92 0EJ. 6.30pm start.
Travel and directions:
The Fellowship Hall is conveniently located close to Sutton Coldfield town centre and therefore has a range of bus routes passing by it and Sutton Coldfield Rail Station in close proximity. A small car park surrounds the hall, however, there is ample public Pay and Display parking only a short distance away.
The Khidmat Centre is easily accessible from Birmingham city centre and it sits on the route for the number 58, 59, and 60 buses. Small Heath train station is also nearby.
The Motorcycle Museum is located directly on the J6 island of the M42, directly opposite the NEC. It is based around a 10-15 minutes walk from Birmingham International Railway Station and the 900 bus which runs from Birmingham to Coventry goes directly past the museum. There is also plenty of onsite car parking available.
You can also tell the CQC about your experience of care at the Trust at any time online at www.cqc.org.uk or by telephoning: 03000 616161.
This Neonatal Safety Application (App) has been developed by Heart of England NHS Foundation Trust (HEFT). It is an electronic resource designed for use at the bedside by registered practitioners. It contains key information, flowcharts and tables designed to help practitioners to deliver safe, reliable evidence based care at the point of care. The App contains essential information extracted from HEFT and Network Policies and Guidelines. Content is based on top safety issues and frequently used policies and guidelines in the HEFT Neonatal Units.
When infections spread in hospitals this always tends to make headlines. We have seen a number of serious infections spread in hospitals over the past couple of decades including Clostridium difficile, an infection that can cause serious gastrointestinal infections, as well as blood poisoning or endocarditis (an infection of the inner lining of the heart). There is also MRSA, a bacterial infection that can also cause minor wound infection.
To anyone reading about it, an event like this can seem incredibly alarming, particularly where the infection has serious symptoms or can cause death. In recognition of this, over the years steps have been taken to try and minimise or avoid infection outbreaks in hospitals, but are they effective and do we really have infection under control?
Management of infection in 2013 for hospitals means acknowledging the risks that are presented and taking steps to prevent them. Often, the bugs that cause infections are spread by skin-to-skin contact, from objects, surfaces, food and water so Hospitals will have a strict dress code and good hand hygiene that all staff will practice.
Sterilisation, disinfection and regular cleaning are all also part of the infection control practice most hospitals undertake, with equipment regularly sterilised and wards and waiting areas cleaned as often as possible. If risk of an outbreak of an infection is looking like it could be on the horizon, steps are then put in place to ensure quick isolation and treatment of anyone who has become infected.
It is important for patients and visitors to Hospitals to also be aware of the risk of spread of infection particularly for those patients who are already vulnerable.
Some simple steps can be followed to keep the risk of infection to a minimum. Firstly, keeping your hands clean is the best and easiest way of stopping germs from being passed from one person to another. So follow simple steps such as washing your hands before meals and after using the toilet. If you have had a bug such as norovirus, please try to avoid visiting hospital until at least 48 hours after your last symptoms, because it can spread very easily and will have a far greater effect on those who are already sick.
During a Hospital stay, as well as keeping good hand hygiene, bugs can also be kept at bay by ensuring that you do not share any flannels or towels and that any clothing including bed clothes and dressing gowns are washed seperately at a high temperature.
There are ongoing risks of infection for any Hospital, simply because of the nature of being a centre for treating the sick. However, when proper precautions such as the ones mentioned are taken, it is a fairly simple and straightforward matter to ensure that we keep infection under control.
To find out more about infection prevention and tips on hand hygiene, follow @majorhandwash on twitter.
 The Trust’s response to recent media stories, 22 October 2013:
The Trust’s response to recent media stories, 22 October 2013:
Sue Moore, managing director for Good Hope Hospital, said “Good Hope delivers a wide range of surgery and we plan for this to remain the case in the future with strengthened and robust emergency medical services and specialist surgery.
“Service reviews, led by senior clinicians, are regularly undertaken in order to determine how best to meet the needs of our patients, now and in the future. It is important we look at potential options for doing things differently, because healthcare continues to change with advances in clinical practice.
“No decisions about any service changes have been made, as we are still at an early stage of appraising a number of potential options which have been developed over recent months. No changes to surgery would be made without extensive engagement with GPs and patients; and would be based on meeting Royal College standards and improving outcomes for patients.
“We expect to be in a position to share the options in early 2014, but can confirm we are totally committed to building a sustainable future for surgery at Good Hope to deliver the safest and best care possible to our patients. In fact there is potential to develop centres of excellence for a number of surgical specialties and therefore to treat patients from a wider geographical area.”
If you’re about to visit someone in hospital then give some thought to making sure your visit is a positive experience for you and those around you. This means understanding the requirements with respect to the spread of disease and hygiene, and sticking to the rules that the hospital has put in place for the benefit of the patients. Here are some tips on how to get hospital visiting right:
1) Don’t visit the hospital if you’re unwell. Many of those in hospital have severely weakened immune systems, which makes them much more vulnerable to any germs or bugs you might bring in with you. No matter how much you might want to visit someone, if you’re not well then the best thing you can do is to stay at home until you’re better.
2) Hand hygiene. Germs and disease can be spread via touch, so careful hand hygiene is important for all visitors, both to make sure you don’t pass anything on, and so that you don’t pick anything up. Wash your hands with soap and water when entering and leaving the hospital, and when going in or out of the patient’s room – or alternatively use alcohol rub each time.
3) Be aware that other patients might need rest. Patients who are ill enough to be in hospital are likely to get tired very quickly so have some consideration for those around you, as well as the person you’re visiting. Try to keep the noise levels low, don’t visit in large numbers and don’t play music or bring strong smelling food with you.
4) Call in advance to make sure you are aware of ward closures and visiting times. It may not be particularly convenient for you to have to time your arrival with hospital visiting hours, rather than when it works for you, but if you don’t arrive at the right time then you could find that you won’t be able to visit. Make things easier for everyone and find out when visiting times are – then don’t overstay your welcome.
5) Should you bring presents? It’s lovely to receive a gift when you’re sick in hospital so by all means bring the traditional presents of chocolate, sweets, magazines, fruit or books. Avoid anything that might cause a nuisance and if you want to take flowers then it’s a good idea to check with the ward staff first.
Visiting someone in hospital can make a great difference to their experience, as they will feel supported and cared for – as long as you do it properly. If you have any doubts or questions don’t hesitate to contact our Patient Services team on 0121 424 08 08.
Locals looking for a greater awareness of two of the most common cancers among women are invited to attend a talk at Solihull Hospital next week.
With ovarian cancer being the nation’s most common gynaecological cancer and around eight women diagnosed with cervical cancer each day; Solihull Hospital consultant gynaecologist, Raj Saha, will be giving Silhillions the chance to learn what to look out for and ask any questions about these conditions.
Mr Saha says: “The stage at which both ovarian and cervical cancer is diagnosed plays an important part in determining the outlook for women with the disease. If diagnosed early, the effectiveness of treatment will usually be very good and a complete cure is often possible. Anyone who wants to learn more about these conditions is welcome to come along to this free event at the Hospital..”
The health talk is taking place on Thursday 24 October at 5pm in the Education Centre at Solihull Hospital. To book your place or to find out details of the Hospital’s future health seminars, contact Sandra White on 0121 424 1218 or email sandra.white@heartofengland.nhs.uk.
A patient at Heartlands Hospital has received the prestigious ‘Robert Lawrence’ medal from Diabetes UK in recognition of 60 years’ triumph over the condition.
Gillian Tait, aged 77 from Birmingham, was diagnosed with Type 1 diabetes when she was 15 years old. She currently injects insulin twice a day and estimates that she has injected herself around 45,000 times over her lifetime so far.
Having diabetes has not deterred Gillian from living a full and energetic life. Over the years, she has enjoyed folk dancing, rambling, gardening, a full-time job as an infant teacher and has continued to advise and support other diabetics. Gillian has also worked hard to raise awareness of the condition through membership of the diabetes association committee.
Gillian said: “Managing my condition is a lot easier now than it was to begin with. When I was first diagnosed I used to weigh everything I ate and wrote the food values down, but then I got used to being able to judge this for myself.
“When I was diagnosed with diabetes I was told insulin would extend my life by 15 years so I thought I would live until I was thirty years old. This spurred me on to do everything I wanted in life, so I went to college and trained as a teacher and took up all the hobbies I wanted to do.
“Now I’m 77 and insulin is my friend – I’m glad to have it and it makes me feel well. I’ve been very careful and followed all the instructions given by the doctors and nurses to keep me on track, so I’m very proud to have received this medal. I hope that it gives other diabetics hope that they can live a fulfilling life. I’m very thankful to Dr Rahim, Dr John and the team at the Heartlands Diabetes Clinic where I have been a patient for many years.”
Diabetes specialist, Dr Reggie John, said: “Gillian has taken good care of her diabetes and is an outstanding example of the fact that diabetics can have a normal life, if the compliance is good.
“Successful control of Gillian’s diabetes should serve as an encouragement not only to her, but to all newly diagnosed diabetics.”
The Robert Lawrence medal is named after Dr Lawrence, one of the first people in the UK to receive insulin when he was diagnosed in the 1920s, and a founding member of the British Diabetic Association, now Diabetes UK. Each year, the medal is awarded to someone who has lived with diabetes for 60 years.